States are failing to adequately test children’s blood for lead exposure, according to a recently released study by the Public Health Institute in California. Vast numbers of U.S. children who may have been exposed to lead are going undiagnosed and remain vulnerable to the long-term, harmful effects of the neurotoxin.
Nationally, only two out of three children with elevated blood lead levels were tested and identified by medical providers. Based on estimates, under-testing by pediatric care providers appears to be “endemic in many states,” according to the study Assessing Child Lead Poisoning Case Ascertainment in the US, 1999–2010. The shortcomings are particularly notable in the Southern and Western United States.
The Public Health Institute’s researchers estimate that during the period that was studied, from 1999 to 2010, 1.2 million cases of elevated blood lead levels among children under 6 are believed to have occurred, but only half of those were reported to the Centers for Disease Control and Prevention.
In some states, as many as 80 percent of lead-burdened children were not diagnosed at all.
The study also found that:
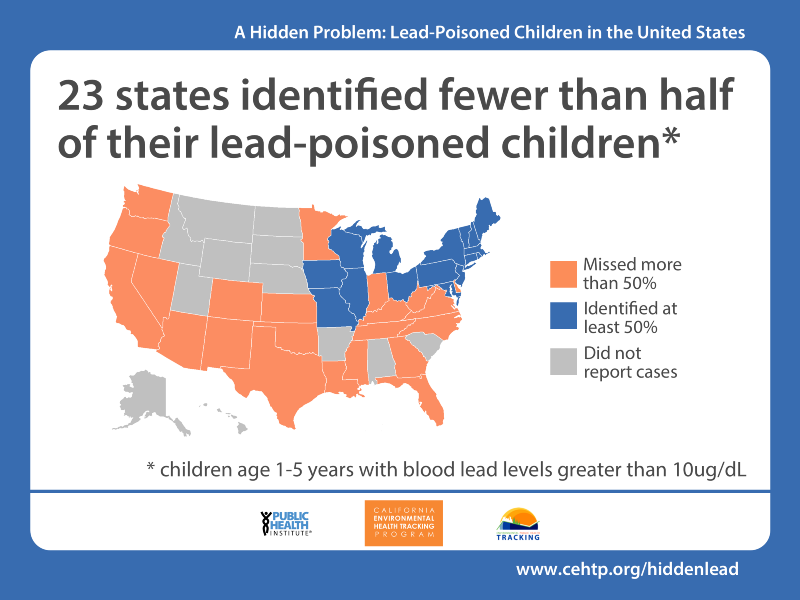
- More than half of children with elevated blood lead levels were not identified in 23 of 39 states where data were available.
- Although the greatest numbers of reported cases were from the Northeast and Midwest states, based on the study’s prevalence estimates, the largest number of cases occurred in Southern states.
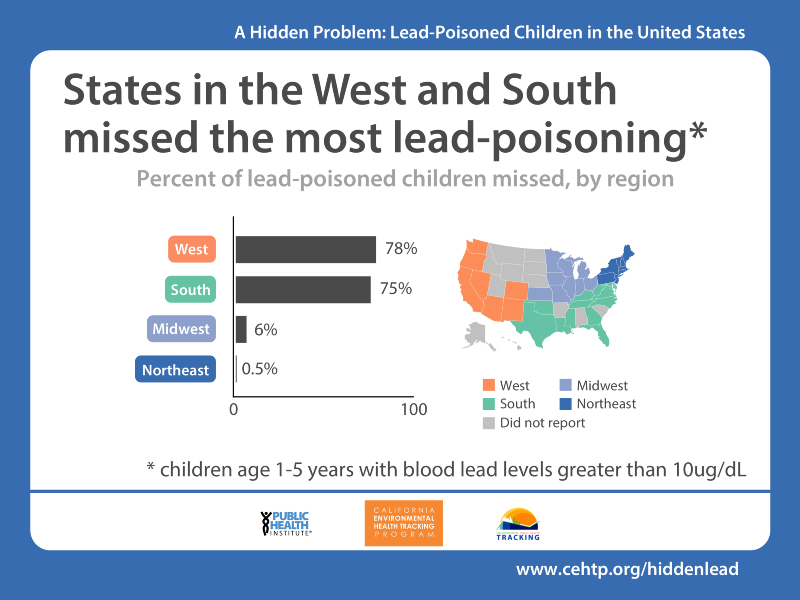
- In Southern and Western states, about three times as many children with elevated blood lead levels were missed and not diagnosed.
- In California, the study estimates, only 37% of children with elevated blood lead levels were identified.
“The numbers of children with lead poisoning we know about are already frighteningly high — especially since lead poisoning is preventable,” research scientist Eric Roberts, a co-principal investigator of the California Environmental Health Tracking Program at the Public Health Institute, said in a statement.
“But now we know that many more children who have been exposed to lead are not tested, not counted and not treated. Without the true numbers, we can’t help the children who have been poisoned, or root out how and why so many children are being poisoned in the first place.”
The study confirms what some of the nation’s leading experts have long suspected: that childhood prevalence rates don’t accurately reflect the real number of lead-poisoned children because they aren’t being properly screened, tested, and diagnosed.
“I would like to think there’s going to be more discussion moving toward more aggressive testing, which might be considered universal testing. At the very least we could enforce the law as it is now or convince clinicians to behave in accordance with it,” Roberts said in an interview with ThinkProgress.
The Centers for Disease Control and Prevention has stated that no level of lead in children is safe, and experts have emphasized that primary prevention is essential to eliminating the threat of lead exposure.
Scientific research on the neurotoxic effects of lead on the developing brain has shown that elevated lead levels can cause a host of lasting damages: increased aggression, lack of impulse control, hyperactivity, inability to focus, and delinquent behaviors. A growing body of evidence has shown that lead in the bloodstream—even at low levels—is associated with lowered IQ levels, attention-related behaviors, and poor academic achievement in children.
“The numbers of children with lead poisoning we know about are already frighteningly high.”
Childhood blood lead tests are required by law for children on Medicaid, a federal/state health care financing program for low-income families. But the federal government has long known that compliance rates are low. One 1999 report compiled by the U.S. General Accounting Office found that despite the federal testing requirements, “most children in or targeted by federal health care programs have not been screened.”
The report found that for almost two-thirds of children under the age of 6, whom the CDC identified in a national survey as having elevated lead levels, the blood lead test conducted as part of the survey was the first such test the children had received. The GAO found similar low screening rates in other federal health program data, and additionally found that “screening rates vary greatly from state to state and locality to locality.”
More recent Medicaid data suggests that in 2015, only about 38 percent of children ages 1 to 2 had blood lead screening tests, according to a Department of Health and Human Services bulletin released last year.
A better way to test for lead exposure
University of Cincinnati Professor Kim Dietrich, who has spent decades researching the impact of lead on children’s health and behavior, peer reviewed the study, which was published last week in Pediatrics, the journal of the American Academy of Pediatrics.
In an email, Dietrich said he was not surprised by the results.
Dietrich led a groundbreaking study published in 2008 that examined the long-term effects of lead exposure on a group of Cincinnati children, and provided the first evidence that children exposed to lead in the mother’s uterus or during early childhood have an increased risk for criminal behavior later in life.
Finding environmental sources of lead is key to preventing childhood lead exposure, says Dietrich, but it’s also important to enforce targeted screening for children living in high-risk areas, he said. Low-income, urban neighborhoods, particularly those with homes built before 1978 (when the federal government banned lead from paint in residential homes), fall into this high-risk category.
Dietrich recommends that for children in these areas, blood testing begin at 6 months, when a baby starts crawling or becomes ambulatory, followed by testing at 12 months, 24 months, and 3 years of age.
“That should be as done as faithfully as we try to do vaccination immunization. It should be part of the medical regimen for children,” Dietrich, director of epidemiology and biostatistics at the university’s College of Medicine, said in an interview.
Misconceptions about kids’ lead exposure are regional—and systematic
States mistakenly assume that children are not at risk based on previous testing data and assumptions about high-risk factors. For example, Midwestern and Northeastern states are perceived to have older housing and therefore more children at risk for lead exposure. But Roberts found that the California has higher rates than the nation as a whole when it comes to the percentage of children under the age of 6 living in pre-1978 housing.
“Well, of course we always thought it was a Northeast/Midwest problem, because in those states the physicians think it’s a problem so they test more and they find [the children],” said Roberts.
Researchers created a model to calculate the number of lead exposed children and found that although the Midwest and Northeast have the greatest number of children with elevated blood lead levels who were reported to the CDC, the greatest number of cases occurred in the South. And although the West had the smallest number of cases, this region also had the greatest proportion of missed cases (89 percent).
Roberts, a pediatrician, said the anecdotal evidence he’s gathered over the years in California indicates that pediatricians in California don’t screen for childhood lead exposure because they believe children aren’t being exposed to lead. When he asks the pediatricians how they know this, the pediatricians tell him it’s because they’ve “never had any kids test positive.”
“It does appear to be the sort of circular argument of: if we test then we see it’s a big problem and so we test. And if we don’t test, then we don’t think it’s a big problem, so we don’t test,” said Roberts.
It’s one of the reasons Roberts decided to dig into the question of how to accurately count the number of children being exposed nationwide. Most states, he said, instruct pediatricians to test children who are at risk, but many doctors don’t have the proper training to determine this, he said. Couple that with preconceived notions about what communities are burdened with lead and this results in an echo chamber—pediatricians don’t test and public health agencies receive data that is not accurate, said Roberts.
“So the idea becomes that you’re supposed to turn to your state department of public health to tell you what communities are at risk,” said Roberts. “State departments of public health are taking the clinical data, repackaging it and passing it back to the clinicians, and saying: ‘See we’ve never found any lead; you’ve never found any lead poisoning so there must not be any.”
