Sen. Ron Johnson (R-WI) omitted key facts at a hearing Wednesday in his attempt to highlight Medicaid’s role in fueling the opioid crisis. The Homeland Security and Governmental Affairs Committee, which he chairs, released a report the same day, drawing connections between the public insurance program and opioid epidemic.
Johnson asked his staffers to investigate the relationship and draft a report after he read an anecdote from journalist Sam Quinones’ 2015 book “Dreamland: The True Tale of America’s Opiate Epidemic.” Quinones wrote, “For a three-dollar Medicaid co-pay … addicts got pills priced at thousands of dollars, with the difference paid for by U.S. and state taxpayers. A user could turn around and sell those pills, obtained for that three-dollar co-pay, for as much as ten thousand dollars on the street.”
The report found about 1,000 instances between 2014 and 2017 in which Medicaid insurance was improperly used to obtain prescription pills and, in some cases, was illegally resold. This was, according to Johnson, more pronounced in states that expanded Medicaid eligibility through the Affordable Care Act (ACA).
The report fails to include how Medicaid fairs with other insurance types. It mentions preliminary research into opioid-related Medicare fraud but makes no mention of private insurance.
Moreover, the report draws connections between Medicaid and the opioid epidemic in an insular way and negates how various players in the health care system — doctors, pharmaceutical companies, etc. — contribute to this evolving crisis, which accounted for 64,000 overdose deaths in 2016 and helped shorten life expectancy for a second consecutive year.
“I do not believe that Medicaid should be singled out in this regard,” said Andrew Kolodny, co-director at the Opioid Policy Research at Heller School in Brandeis University, during the hearing.
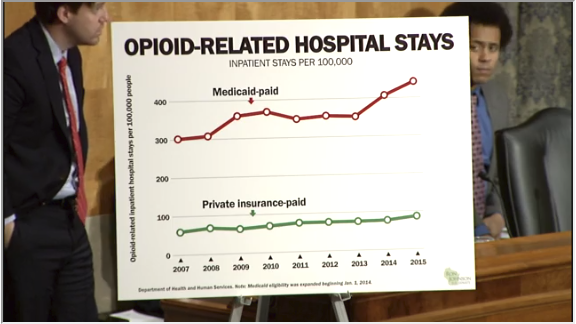
But Johnson did just that, stressing his point through a misleading chart during a Q&A with Kolodny. He asked Kolodny to react to data from his report, which Johnson likened to Kolodny’s own chart presented moments before.
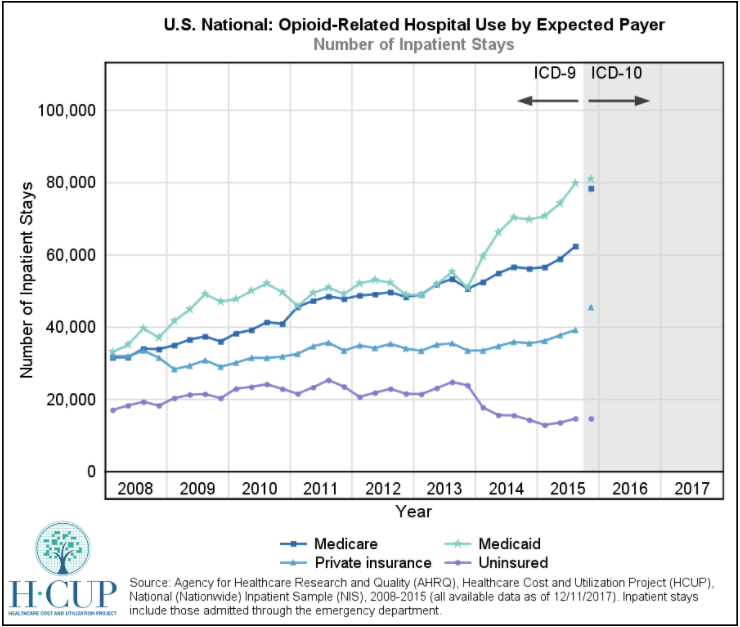
“We actually developed this off the hard numbers,” Johnson said. His chart, below, shows opioid-related hospital use by the expected insurance provider:
But this is the complete chart, which Johnson cites but alters in his report, provided by Healthcare Cost and Utilization Project:
“It’s misleading to only select Medicaid and private insurance,” Rebecca Haffajee, assistant professor at the University of Michigan’s School of Public Health, told ThinkProgress. “All four rates are increasing for all four populations.”
While the public tends to look at the rising mortality rate as an effect of the opioid crisis, it’s important to also look at hospital stays. “For every death there is a thousand hospitalizations — hospital stays,” said Haffajee. Johnson’s skewed chart doesn’t present a convincing case for the “deluge of victims” (Johnson’s words, not Haffajee’s) on Medicaid insurance, she added.
When speaking of hospitalizations for opioids — heroin included — in a recent Health Affairs report, Kolodny said, “What we saw in that chart was a very significant rise for all payer types including self-pay. And what we saw in the Health Affairs paper — we saw a substantial increase for Medicaid, but an even greater increase for Medicare.”
Johnson took Kolodny’s point and added, “all we did was just take [federal data] and put it to number per hundred thousand just to make it more a little bit relatable.” But that’s not all he and his staff did; he used incomplete data to produce a report and justify his hearing.
“Opioid overdoses have been increasing in people with all types of insurance and in people from all economic groups, from rich to poor,” said Kolodny earlier in the hearing. While it’s important to understand how insurance companies play into the nonprescription of opioids, it’s also important to point out the role of insurance in covering addiction treatment.
Haffajee said Medicaid is fairly generous, and the plans cover at least one of three types of medication-assisted treatments — the gold standard of care — in all 50 states. “Sometimes [we] might see adverse outcomes, not because insurance causes this, but [it] has to do with life conditions,” she said.