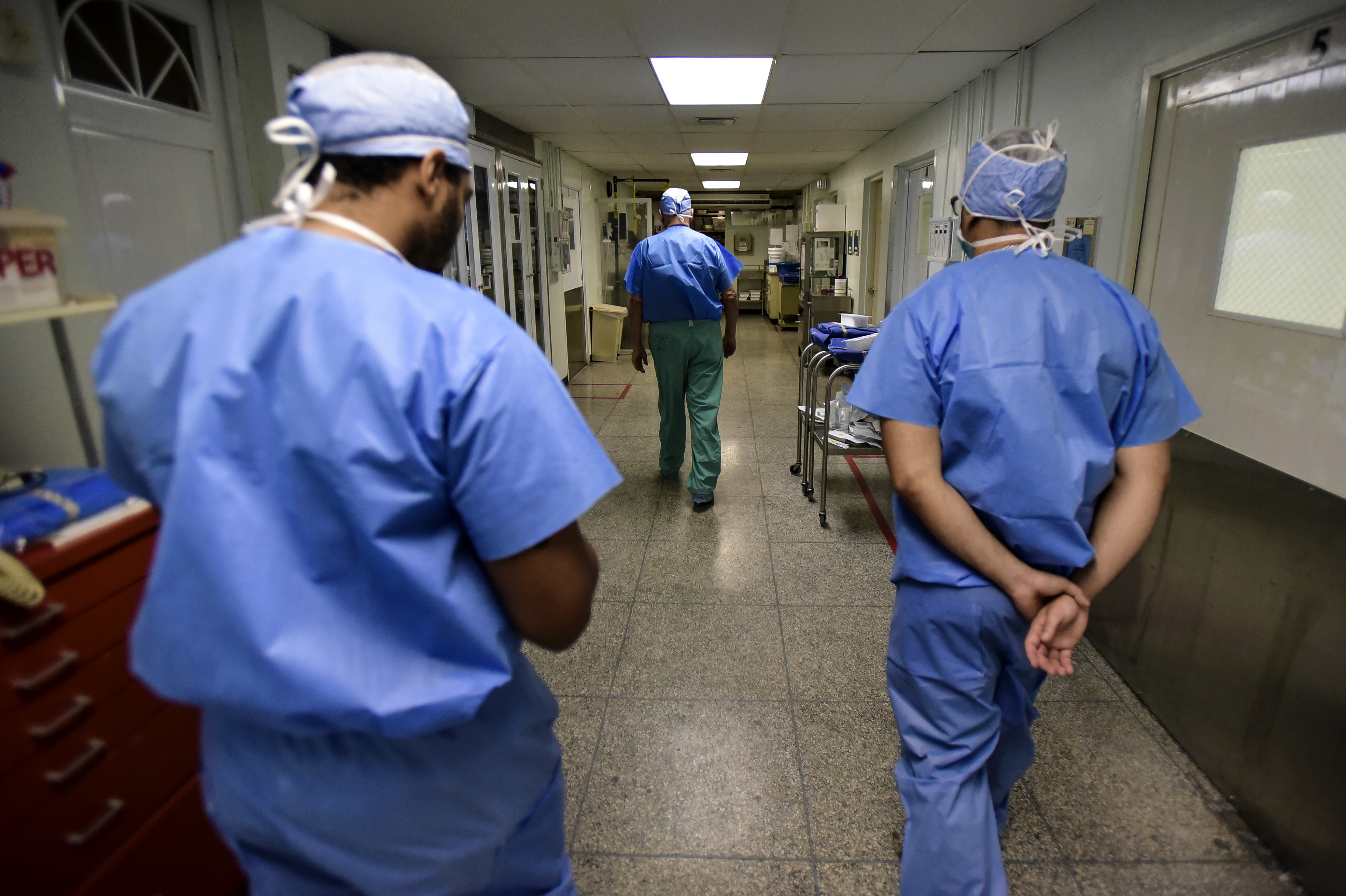
Just three months ago, Hurricane Harvey made landfall on the Texas Gulf Coast. The hurricane took at least 88 lives; more than 311,000 housing units were damaged; and the state is just beginning to understand the hurricane’s health toll.
Add another caveat to recovery efforts: critical health care programs that serve Texas’ most vulnerable face financial uncertainty.
Congress failed to renew funding for federally qualified community health centers and the Children’s Health Insurance Program (CHIP), thus threatening the stability of a health infrastructure setup for the poor. Texas isn’t the only area where uncertainty exacerbates ongoing recovery efforts. Puerto Rico’s clinics and CHIP program face a funding cliff too.
Congress missed a critical deadline to reauthorize new funding for the centers and CHIP on September 30. Centers provide medical care to low-income persons in undeserved areas and CHIP provides insurance to children from modest-income families. Already, one of the six federally-funded clinics in Delaware closed last week because Congress failed to commit to 2018 funding. Westside Family Healthcare Spokesperson Maggie Norris-Bent said some patients, served by the Middletown clinic that closed, now need to travel an extra 15 to 25 miles for care. Colorado officials warned CHIP families by mail last week that the program will end January 31, 2018 if Congress doesn’t act.
Texas and Puerto Rico’s community health centers are playing an especially critical role right now, as there’s been a spike in demand post hurricanes.
“By statute, we provide care to people in need” regardless of their ability to pay for it, said Amy Simmons Farber, spokeswoman for the National Association of Community Health Centers. And centers are facing a lot of anxiety right now, she added.
Seventeen Texas health centers — half of which serve Harvey-affected residents — will immediately be impacted if Congress does not renew funding.
“We are facing a ticking clock and a crowded [congressional] legislative agenda,” said Simmons Farber. “We need action this month … if Congress does not act, our understanding is that hundreds of health centers with budget periods starting in January will experience major shortfalls.” A loss of federal funds will lead to hiring freezes, staff layoffs, or clinic closures. There are over a thousand clinics that receive federal funding, and they serve 27 million patients nationwide.
Seventeen Texas health centers — half of which serve Harvey-affected residents — will immediately be impacted if Congress does not renew funding by December 31st, said Jose Camacho, the executive director of the Texas Association of Community Health Centers. There are 76 centers total statewide; some have various sites. This funding accounts for 27 percent of the overall funds. Without this, come January 1st, hiring freezes for admin and providers are inevitable.
“We can’t have interruption of services, so what do you do?” Camacho said. “Employees are aware of these challenges. Folks need their jobs. They are going to be unfortunately looking elsewhere … What do [clinics] tell providers that want to come work for them? How do you answer the question ‘do you have stable funding’?” This will take an operational toll, meaning longer wait times for patients, he added.
Texas has the highest uninsured rate nationwide at 16.6 percent. Forty-two percent of patients that Camacho’s centers serve are uninsured, meaning clinics can’t bill an insurance company for medical care. Six to seven percent of the people who walk in are covered by CHIP. “That program is sending termination notices on December 22” — days before Christmas — if Congress doesn’t renew funding, Camacho said, potentially adding to the number of uninsured.
Statewide, CHIP covers 400,000 children and pregnant women. Texas Governor Greg Abbott requested $90 million dollars from the Centers for Medicare and Medicaid Services (CMS) to keep the program open through February. If CMS doesn’t provide the stopgap funding, CHIP will end on Jan. 31, 2018.
Harvey devastated some Texas clinics. The Port Arthur prefabricated clinic made it through the hurricane but once they lost power, thieves damaged the clinic while stealing drugs. Likewise, the Houston clinic was operational until officials subsequently discovered mold. And the clinic in Katy flooded when heavy rain struck. Now, any measures meant to prevent future damage are paused as funding is uncertain.
One in 13 people nationwide depend on centers for care. In Puerto Rico, one in 10 people depend on these centers. Elevated poverty and unemployment means that residents heavily rely on the centers. Like Texas, the centers were hammered by hurricanes, and are still recovering.
As of Oct. 20th, 83 out of 93 clinic sites are open, but open does not mean sites are operating like they were before Hurricane Irma and Maria hit nearly three months ago, according to Geiger Gibson of RCHN Community Health Foundation research.

Director of U.S. programs at the nonprofit Direct Relief, Damon Taugher, who was last on the island a month ago providing aid, said you cannot overstate centers’ role right now. In addition to providing dental, primary, and behavioral care, centers are providing ambulatory care — care that’s typically given in emergency rooms.
One center had to spend $50,000 on diesel fuel.
“They are providing a wider range [of] services even under financial constraints,” said Taugher. The nature of a community center is to give what the community needs and so they’ve even been providing food and water. “They’ve been tapping into groups like ours” to meet residents’ needs said Taugher. His or ganization has donated millions to federally qualified community health centers in Puerto Rico.
Some centers are supplying this aid all while operating on generators to keep the doors open. One center had to spend $50,000 on diesel fuel — a cost the site could not have budgeted for, Taugher said.
Precarious funding is especially dangerous as 83 percent of operational revenue comes from the federal government, specifically Medicaid/CHIP and grants. (Congress failed to reauthorize the latter.) Historically, Puerto Rico’s health infrastructure has suffered due to lack of adequate funding. And Puerto Ricans report poorer general health compared to mainland residents, and see higher rates of diabetes and heart disease.
The only silver lining is — unlike the other four U.S. territories that will exhaust their CHIP funding by the end of December — Puerto Rico’s program is projected to run out of money in March 2018. CMS stopgap funds keep the program operating an extra three months. Roughly one in two Puerto Ricans are on Medicaid/CHIP; 89,372 residents are enrolled in CHIP.
The funding cliff is a concern, said Taugher. “But I think there are so many things to work through in the community. This is another layer of that — they are having to deal with in addition to everything else.” Electricity is occupying the minds of everyone here, he said. Three months later, people are still asking: “when will we have power?”
This post has been updated to specify that 27 million people are served by community health clinics nationwide and that there are a total of 76 centers in Texas.