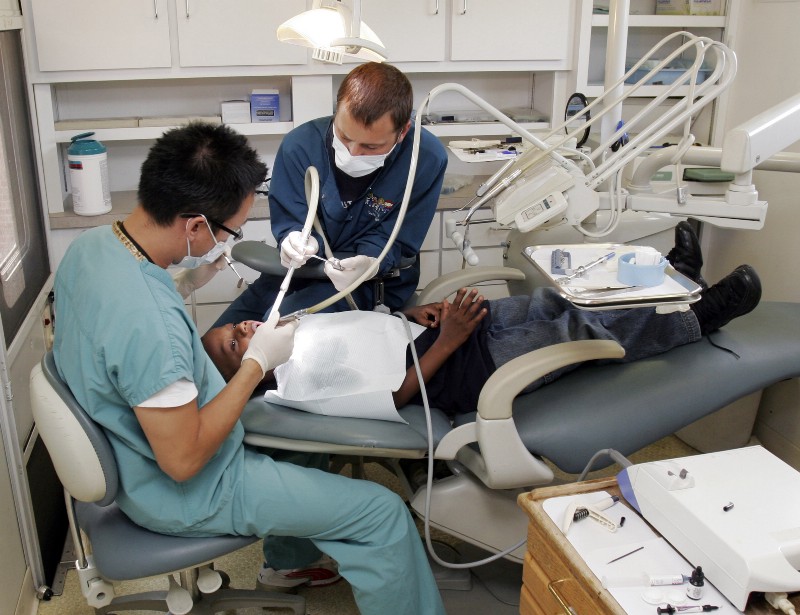
Americans living in parts of the southern United States — areas often burdened with disproportionate crime, poverty, limited health care, and poor schools — will likely live fewer healthy years post-retirement compared to their counterparts in other regions, according to a Centers for Disease Control and Prevention (CDC) report released last week.
CDC researchers analyzed census data between 2007 and 2009, collected death certificates, and conducted telephone surveys during which respondents described their health. The report showed that while Americans on average enjoyed 14 years of good health after retiring, residents of southern states spent many of their final years in and out of emergency rooms and clinics. According to the report, Mississippi, Kentucky, West Virginia and Alabama had the lowest numbers for life expectancy and healthy life expectancy. Black people also fared worse across the board, with a life expectancy that averaged three years less than that of whites.
The trend is obvious throughout what has been dubbed the “poverty belt,” where more than one in three people live in high-poverty areas:
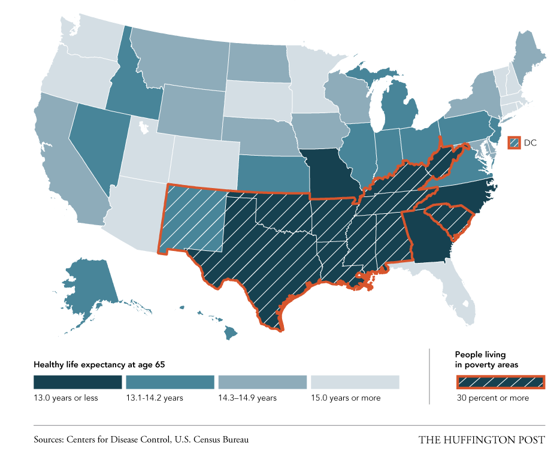
“Where you live in the United States shouldn’t determine how long and how healthy you live — but it does, far more than it should,” said CDC Director Tom Frieden in a press release last week. “Not only do people in certain states and African-Americans live shorter lives, they also live a greater proportion of their last years in poor health. It will be important moving forward to support prevention programs that make it easier for people to be healthy no matter where they live.”
The report underscores a health care battle well underway in numerous states. Nearly a year after the rollout of the Affordable Care Act (ACA), also known as Obamacare, governors in 24 states — including six southern states — still haven’t expanded Medicaid benefits to more than five million Americans, many of whom live in states along the southern poverty belt and suffer from obesity, diabetes, heart disease and other life-threatening illnesses.
While staunch opponents of Medicaid expansion contend that the policy takes a toll on state budgets, there’s some evidence to the contrary. The federal government allocates generous funding for states that choose to expand their public insurance programs. In April, the Congressional Budget Office estimated that states would spend less than two percent more on Medicaid and the Children’s Health Insurance Program, also known as CHIP, because of the ACA. Medicaid expansion can also help generate millions of dollars in revenue by creating more state jobs.
And recent studies published in Oxford’s Quarterly Journal of Economics and the New England Journal of Medicine tell another side to the story. According to that research, Medicaid expansion improves access to care after one year, improves overall health status within two years, and saves lives within five years.
Southern states are already seeing some of the consequences of rejecting the expansion. In Mississippi, the rate of uninsured people jumped by three percent — more than 137,000 people — because Gov. Phil Bryant (R) refused to expand Medicaid. Representatives of the Alabama Hospital Association recently reported that Gov. Robert Bentley’s reluctance to expand Medicaid may have resulted in the shuttering of a dozen rural hospitals in the state.
While people living in states without Medicaid expansion have incomes below the poverty line, they do not qualify for traditional Medicaid benefits, often doled out to low-income parents, children, and people with disabilities. Although many of them consider themselves healthy, according to data collected in a Kaiser Family Foundation data set, one medical emergency can threaten their financial security and that of the country’s.
Rep. Steve Cohen (D-Tenn.), a member of the 33-member Congressional State Medicaid Expansion Caucus, summed up his frustration with recalcitrant governors in a statement to the press last week.
“By not expanding Medicaid, governors around the country — and at home in Tennessee — are conveying a message that they have little concern for the neediest, sickest, and most desperate of their constituents,” said Cohen. “While this may not be Governor Haslam’s intention, the reality of the situation is that 234,000 of our state’s most needy are going or will go without the health coverage that they need and that President Obama’s health care reform law says they should have. Studies have even shown that thousands of Americans each year will die avoidable deaths because of lack of access to Medicaid. That is unacceptable.”