The ongoing fight over Big Pharma’s pricing policies continues as congressional leaders shift their focus to a drug that police departments use to treat heroin overdoses. While law enforcement agencies have become more accepting of this approach to combat drug abuse, recent price spikes put the future of city and state distribution programs in jeopardy.
Earlier this week, Sen. Bernie Sanders (I-VT) and Rep. Elijah Cummings (D-MD) blasted Amphaster Pharmaceuticals, the maker of the drug naloxone, in a letter in which the duo questioned the rationale of increasing the price of the drug during a time when heroin overdose deaths have more than tripled within a three-year period.
“Over the past several months, police departments, law enforcement agencies, and public health officials across the country have warned about the increasing price of naloxone, which they use to combat the scourge of heroin abuse,” Sanders and Cummings wrote in their letter.
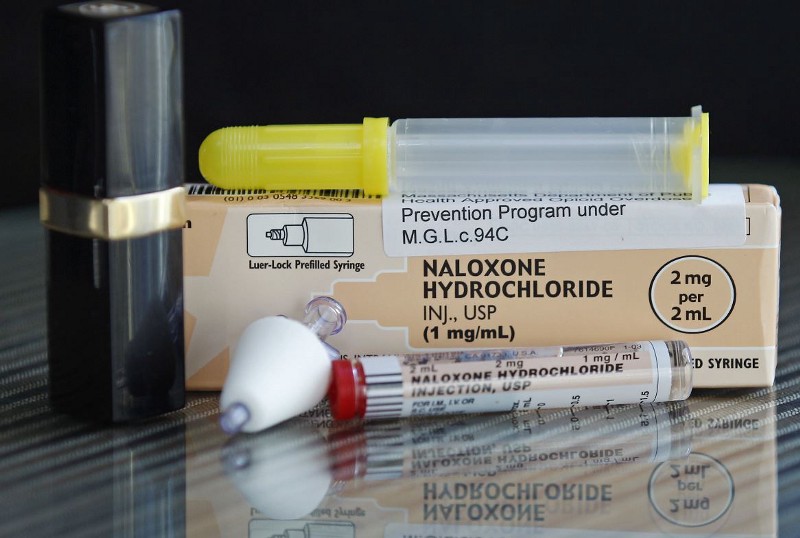
Naloxone, a generic drug that’s also known as Narcan, reverses the effects of potentially fatal opioid overdoses by relieving the depression of the nervous and respiratory systems and quelling symptoms of hypertension. Nearly half of U.S. states have passed laws granting wider access to naloxone, which can be administered in the bloodstream and through the nostrils. Doctors in those states can prescribe naloxone to friends and family members of opioid abusers. These measures also remove liability from people who dole out the drug, including police officers.
In April 2014, the Food and Drug Administration approved Evzio, a user-friendly naloxone injector to the satisfaction of public health officials and advocates. However, a sticker price of more than $400 keeps the tool out of the hands of many people who would prefer having the drug on hand in case a friend or family member overdoses. The price of the formula that can be injected nasally also doubled to the chagrin of law enforcement officials and heads of nonprofits, many of whom have turned to Amphaster — its sole producer — for answers.
“You’re being held at the whim of companies that can do what they want because they have a monopoly on a drug,” Eliza Wheeler, project manager for the Harm Reduction Coalition’s DOPE Program, told MedPage Today in November 2014. “The balance of our program rests on whether we can afford a product. That they can wantonly raise the price is terrifying.”
When it comes to naloxone, this type of price manipulation is nothing new. Pharmaceutical companies have adjusted prices of the drug according to its demand since it appeared on the market in the early 1970s. After the Centers for Disease Control and Prevention declared an opioid epidemic in 2008, for example, the price of the drug — which cost less than $3 per dose at the time — increased by more than $1,100 since then.
Today, law enforcement officers are reeling from naloxone price spikes of up toward 50 percent that threaten the potential to curb heroin addiction. Health officials in Maryland said they’re worried that the rising prices will stall their efforts to train police officers in doling out the drug to those experiencing an overdose. Long before Sanders and Cummings railed against Amphaster, Massachusetts Attorney General Maura Healey inquired about the increase in the price of naloxone amid a public health emergency in the state.
Ed Schneiderman, New York’s attorney general, took a similar approach and secured an agreement for $6 rebate per dose to agencies in the state for a year. Lawmakers, however, aren’t satisfied. In their letter, Sanders and Cummings called on Amphaster to make across-the-board price changes and subsidies similar to what was done for New York consumers, citing its potential to save lives.
“Although we are encouraged by your stated willingness to work with other states, it remains unclear why your company has not already lowered its prices in states other than New York. The rapid increase in the cost of this life-saving medication in such a short time frame is a significant public health concern,” the duo wrote.
Data from the Centers for Disease Control and Prevention supports their point: if made more readily, Naloxone could prevent more than 20,000 deaths in the United States annually. A 2013 study found that distributing the drug could save one life for every 227 kits that are distributed. Empirical evidence has also played a part in authorities’ change of heart. For example, more than 100,000 overdose reversals were reported from 188 naloxone distribution programs in the United States. In these programs, more than 53,000 people had been trained to administer the drug.
That’s why more people want to see community groups get access to the drug during a critical juncture in the fight against heroin abuse. One criticism has been that of the monopoly that pharmaceutical companies have on these products. Years before naloxone’s price exploded, advocates suggested taking the new approach a step further by distributing naloxone over the counter, predicting that failing to do so would further marginalize heroin addicts.
Even though widespread distribution in this manner doesn’t seem likely to happen, discussions about taking the life-saving medicine out of Big Pharma’s hands still occur. The editorial board of The Herald News, for example, suggested that pharmaceutical companies in Massachusetts develop a drug-delivery device that could compete with Naloxone toward the end of last year.
In a twist of irony, John Santilli of Access Market Intelligence, an organization that works with Big Pharma, had similar thoughts about the drawbacks that Amphaster’s stranglehold on naloxone could have for heroin addicts and their families.
“The increase in price of nasal naloxone from the lone manufacturer is having a large negative impact on the ability of community groups to pay for the drug,” Santilli told the Modern Medicine Network last year. “The price of a new auto-injector naloxone is projected to also be expensive. To keep naloxone affordable, it should not be burdened with regulatory obstacles and made available at a price similar to what it costs to produce,” Santilli added.