Over the past year, Dr. Shanthi Ramesh performed abortions for seven sexual assault survivors and she recalls Medicaid insurance only paying for two.
It didn’t matter that they were all technically eligible for Medicaid — meaning, they were all poor enough to receive public health insurance — or that a doctor, in her professional opinion, believed they were raped. She says four of the seven women did not report their assaults to local law enforcement and, so, insurance didn’t cover it. One did try to report, but police didn’t believe her.
In Virginia, a survivor who needs to terminate a pregnancy can tell the provider about either the acute rape or long-standing history of sexual violence during counseling. At some point during this first visit, the patient could also disclose they have Medicaid, typically meaning they earn no more than $16,146 a year (for a household of one). If the patient reports the assault and the provider submits a form to the state health department at least 48 hours before their abortion, public funds should pay for the procedure. At one facility in Richmond, that means between $395 to $1,450, depending on how far along the pregnancy is.
“We talk to patients about their options… — making a police report and having their abortion [be] covered in that way — and I would say the majority of women say something to the effect of ‘I’ve already been through enough. I just want to get it done. I don’t want to have anyone else involved,’” Ramesh, an abortion provider in Virginia, told ThinkProgress.
Under current law, Medicaid is supposed to cover abortion services at least in cases of rape, incest, and life endangerment in Washington, D.C. and 32 states, including Virginia. Yet the intersection of Medicaid and abortion — which are stigmatized as handouts and destroying life, respectively — creates a complicated process, perhaps by design, for providers and patients who just want insurance to pay for a health procedure. Sexual assault survivors aren’t exempt from that complicated process.
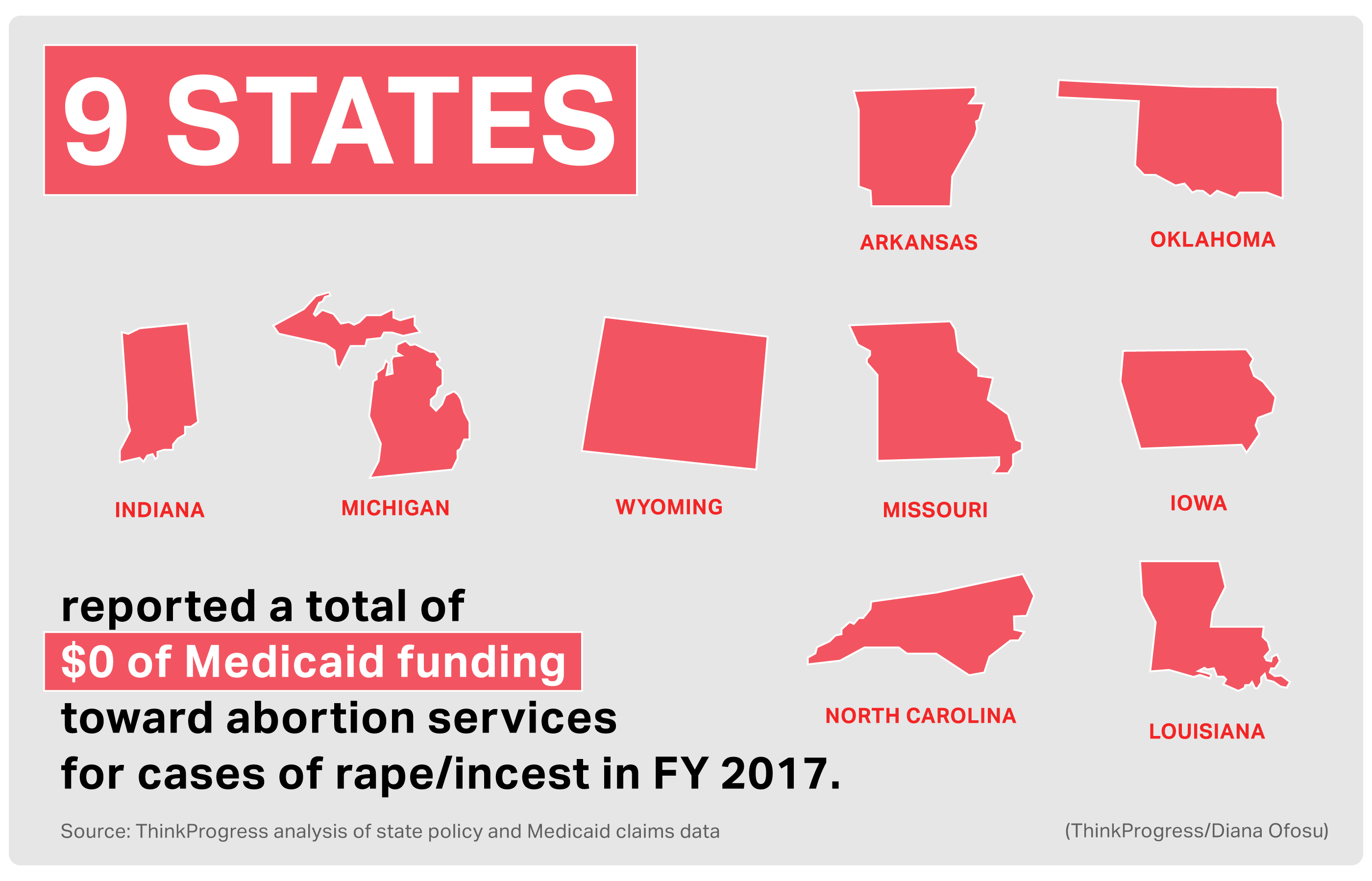
A ThinkProgress analysis of Medicaid claims across the country found few states with coverage restrictions have paid for many low-income people’s abortions — likely due to the bureaucracy, ignorance, or stigma. In fact, in 2017, nine states never paid for a survivor’s abortion and four only paid for one.
“…I’ve already been through enough. I just want to get it done. I don’t want to have anyone else involved…”
In addition to reinforcing a “good abortion, bad abortion” concept, dozens of advocates told ThinkProgress rape and incest exemptions are actually harmful because survivors ultimately aren’t guaranteed to get the health care they need — particularly when it’s conditioned on a police report, as is the case in a few states.
While more survivors are publicly sharing their experiences with rape and assault during this cultural calculus of #MeToo, law enforcement is seldom involved. The statistics say as much: two out of three rapes are not reported to police. There are a lot of reasons why — like feared retaliation or distrust in the criminal justice system — and all depend on the survivor’s life circumstance. Laws generally lack nuance or an understanding of this reality.
“The reality of the way that rape is conceptualized in this country means that women don’t get the care that they need for that rape from the very beginning,” said Dr. Caitlin Bernard, an Indiana provider who performs abortions in hospitals and clinics. “And abortion is just a very small part of that process.”

How we got here
Any restriction on abortion in the Medicaid program begins with the Hyde Amendment.
Since 1976, Congress has excluded abortion from Medicaid’s list of covered services. Lawmakers did carve out some exceptions, permitting federal dollars to pay for abortions in cases of rape, incest, or life endangerment. If states want to cover abortions beyond these exceptions, they have to use their own funding. But most (32 states and Washington, D.C., according to the Guttmacher Institute) generally do not cover abortion beyond Hyde; six of these states also carve out exceptions for impaired fetal growth or physical health of the pregnant person. South Dakota fails to even comply with federal law, permitting public funds only for lifesaving abortions.
In 1998, the U.S. Department of Health and Human Services further clarified these exceptions, telling state Medicaid directors that rape “reporting or documentation requirements may not serve to deny or impede coverage for abortions… [and] any such reporting requirements must be waived… if the treating physician certifies that in his or her professional opinion, the patient was unable, for physical or psychological reasons, to comply with the requirements.”
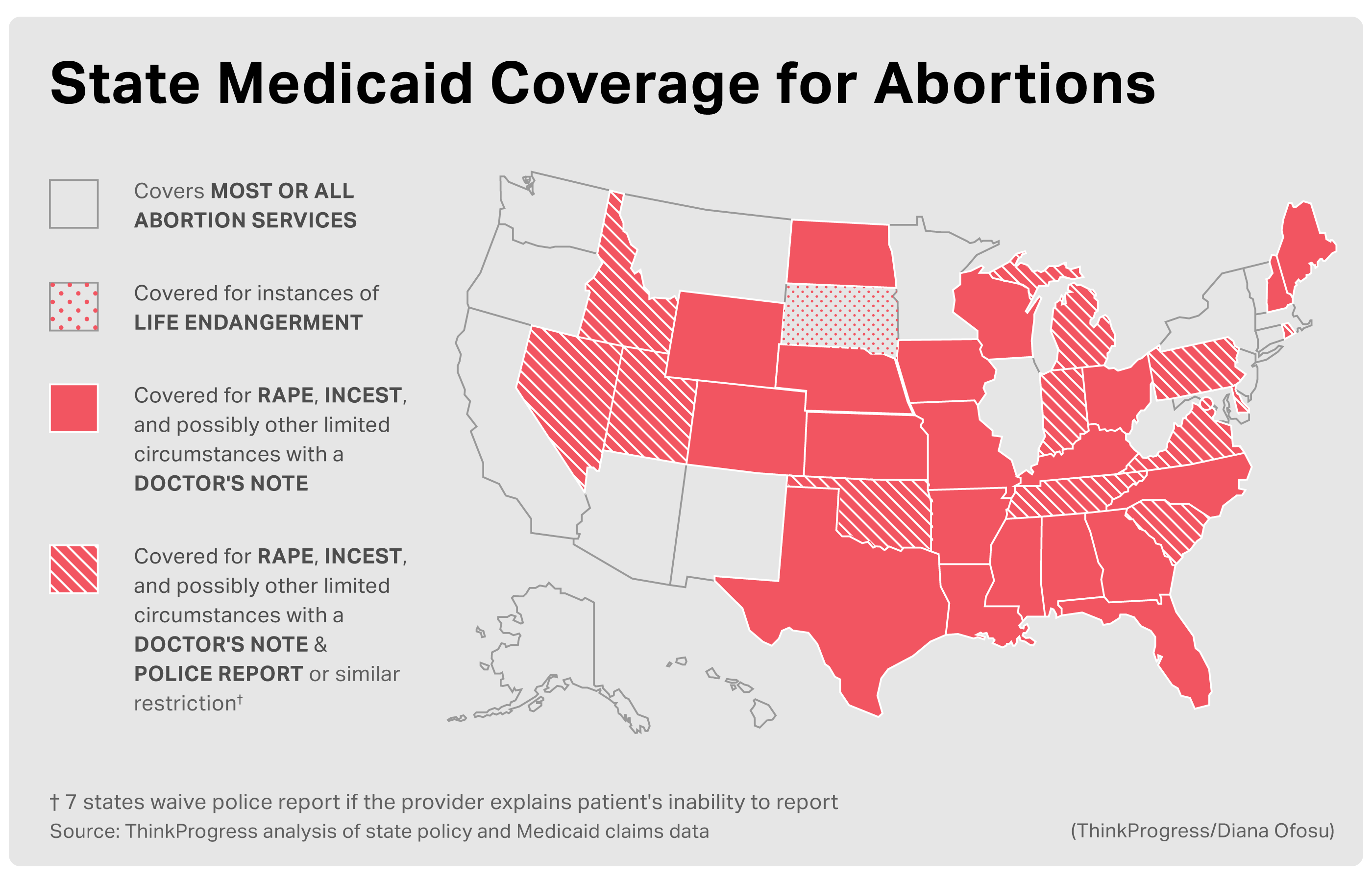
Today, a handful of states still do not explicitly waive the requirement that patients report their rape to law enforcement even if they fear for their lives. ThinkProgress found that at least two states (Utah and Wisconsin) and D.C. only pay for abortions if a police report is filed.
If it’s not a police report, it’s another requirement that’s not widely known and therefore not met. In Virginia, for example, survivors also have the option to report to a public health agency instead of law enforcement, but it’s not a well-known option. When ThinkProgress asked the state’s health department about this option, staff admitted that no one has ever asked. Dr. Ramesh was also unaware of anyone doing so. Tennessee patients can report to police, a public health agency, or a rape crisis center. And Nevada requires an affidavit from both the survivor and provider.
ThinkProgress contacted Washington, D.C. and the 32 states that cover abortion only in those limited situations to see if police reporting or comparable restrictions correlated with fewer Medicaid claims. ThinkProgress asked how many abortions in cases of rape and incest the states paid for and how much officials reimbursed. Just 19 states and the District of Columbia provided 2017 data, eight did not respond, and officials from Colorado and Utah refused to share information, citing concerns that the numbers were so small that releasing information might violate the Health Insurance Portability and Accountability Act (HIPAA). Texas officials wanted to charge more than $200 for the information, and Georgia said it doesn’t collect this data. Ohio didn’t provide the data by deadline and an official cited concerns about the information going public before the midterm elections.
The data shows that most states — with or without police reporting requirements — rarely, if ever, pay for abortions even when their laws mandate it for sexual assault survivors. Neither Indiana, which requires patients to report to either police or the public health service, nor Louisiana, which accepts a doctor’s note as enough proof, paid for any abortions in 2017. Iowa also paid for zero abortions; it requires the governor to personally approve any such payment. Six other states (Arkansas, Michigan, Missouri, North Carolina, Oklahoma, and Wyoming) also said they never paid for an abortion in cases of rape or incest in 2017 and four (Idaho, Kansas, Virginia, and Wisconsin) only paid for one.
Wyoming is the latest state to explicitly waive its police reporting requirement. Local advocates and lawyers with the National Health Law Program (NHeLP) got the state to abide by federal standards beginning in 2018, NHeLP senior attorney Fabiola Carrión told ThinkProgress.
“That might be the reason why it was really difficult for providers to submit a claim,” said Carrión.
Indeed, Wyoming Medicaid has never paid for an abortion when the pregnancy resulted from rape or incest in at least five years.
“But there could be a number of reasons why providers didn’t want to submit a claim: the reimbursement rates are really low, it takes a while, it’s just too troublesome,” she added.
Bureaucracy at work
ThinkProgress’ findings are consistent with expert research. A qualitative study between 2007 and 2010 asked 70 abortion providers in 15 states about their experience billing Medicaid. In 13 of those states, providers reported reimbursement for only 36 percent of all Medicaid-eligible cases.
The problem is, it’s hard to be a Medicaid provider in a lot of these states, said Kelly Blanchard, who co-authored the study.
“In many cases, the Medicaid systems for billing are complex and require a big staff that does billing and interacts with Medicaid — so that definitely was a barrier,” Blanchard, who’s also the president of Ibis Reproductive Health, told ThinkProgress.
When providers are able to get public funds to pay for abortion services, reimbursement rates are usually low. Kansas Medicaid, for example, reimbursed a provider $290 for one abortion in 2017, the state health department told ThinkProgress. But abortions in Kansas can cost anywhere between $600 to $1,675, depending on the procedure.
And when rates are low and reimbursements are slow, “providers just didn’t have the resources to keep fighting the system and would give up,” said Blanchard. “And in many cases the providers would offer discounted services or they would work with local abortion funds.”
Arkansas Planned Parenthood provider Dr. Stephanie Ho noted one colleague has stopped even asking Medicaid to cover abortion services.
“More women who need assistance paying for the abortion — they have easier access to the abortion funds than they would through a Medicaid exception,” she said. Arkansas Abortion Support Network, she noted, doesn’t ask many questions beyond income and household size. For this reason, Ho advises low-income patients to use them because many cite privacy and safety concerns.

The headaches that come with these Medicaid carve-outs motivated activists a few hundred miles north, in Illinois, to get lawmakers to agree to cover abortions beyond Hyde. They were ultimately successful in removing restrictions introduced by their former representative, Henry Hyde; Illinois began covering all abortions on January 1, 2018, with the passage of HB 40.
But problems associated with Hyde linger. Before the bill was passed, a majority of abortion providers weren’t billing to Medicaid at all because it didn’t seem worth going through the cumbersome bureaucracy when there was a strong chance the state would deny the claims. Now, these same providers are having a difficult time setting up a Medicaid billing system, said Brigid Leahy, senior director of public policy at Planned Parenthood in Illinois.
“I’m not sure that there are many more providers out there actually offering abortions or taking Medicaid or covering women who are on Medicaid — that’s because we have to bill on paper,” Leahy told ThinkProgress. “Most Medicaid billing is billed electronically and we did ask the Department to set up a system so that we could bill electronically and have this part of our regular billing system… and they wouldn’t change that, which is really disappointing.”
This is a deterrent for smaller, freestanding clinics who don’t have the means to hire extra staff dedicated to paperwork. No other benefit Planned Parenthood bills to is by paper, said Leahy. It shouldn’t be surprising, as abortion care is often treated differently than other types of health care, she added.
The perfect victim
She was 16 years old with severe developmental delays and was raped. She didn’t know she was pregnant until she was late in her second trimester.
This young girl was the first survivor Dr. Caitlin Bernard had seen since working in the state one year prior. Bernard, a fellow with Physicians for Reproductive Health, is one of the few providers in Indiana who performs second-trimester abortions.
The 16-year-old was covered by Medicaid.
“Nobody that was involved… had any real concept that Medicaid would pay for it.”
“Nobody that was involved… had any real concept that Medicaid would pay for it,” said Bernard. “They were just saying ‘we need her to not be pregnant anymore’ because number one, it’s dangerous for her health and number two, she certainly can’t — is not in a place to be able to parent.”
Indiana should theoretically pay for the abortion, which took place in late August. But even though the rape was reported — in fact, the Indiana Department of Child Services referred the case — Bernard is confident that the hospital will eat the cost of the procedure, as her colleagues have never had Medicaid pay for abortion services. The 16-year-old’s abortion cost somewhere between $5,000 to $10,000, because the abortion wasn’t performed at an out-patient clinic, but in an operating room.
“I don’t have a lot of faith that the hospital will actually be paid for this service,” Bernard told ThinkProgress.
“When it’s only one case a year, then they are able to absorb that cost, but if it becomes more than that, then there’s always the risk that they’ll say that we can’t provide the service since we’re not being paid for it,” she added.
The Family and Social Services Administration for Indiana told ThinkProgress Medicaid has not paid for any survivor’s abortions so far in 2018.
“We have not had any claims for abortion due to rape/incest in 2018 so far that have been reported,” said Communications and Media Director James Gavin by email in October.
If the process hasn’t worked for Bernard’s client, it’s not surprising that it didn’t for others.
“I don’t think our legal system is at all understanding.”
Ramesh, the provider in Virginia and Physicians for Reproductive Health Fellow, was able to get Medicaid to pay for two of her patients. They were all minors, between the ages of 13 and 16, and visited a Planned Parenthood clinic, where she works, as part of a police investigation. Each also had a supportive parent accompany them through the process.
But the other women, all in their mid-20s or early-30s, had to pay for the abortion themselves or with funds raised by non-profits organizations. All but one were also in abusive relationships. As a result, “the idea of going to police and explaining… why this exact sexual encounter that resulted in this pregnancy was rape as opposed to other times” was daunting, said Ramesh.

“I don’t think our legal system is at all understanding,” she said, recalling one patient who was date raped. The patient asked police to come to the abortion clinic with her, but they declined because they decided they weren’t pressing charges.
Virginia has only approved payments for five abortions in cases of rape or incest between 2014 and 2017, according to state data. Ramesh, who’s been a provider in the state for the past year, says she’s seen at least one patient a month who’s disclosed during counseling that their pregnancy resulted from sexual violence. “It’s unfortunately a pretty common experience,” she said. And in 2018, public funds should have paid for at least seven women’s abortions under current federal guidelines — but, as Ramesh’s experience shows, that clearly wasn’t the case.
“For some patients, reporting to the police is potentially empowering for them,” said Ramesh. “But I think to say everyone who has experienced rape and who wants to have Medicaid pay for their abortion has to report to the police is not trauma-informed. I think meeting patients where they are is.”
Whatever the barrier — be it a police reporting requirement for patients or paper billing for providers — low-income people, sexual assault survivors included, aren’t always able to use their own insurance for health care. Of the dozens of experts ThinkProgress spoke to, no one said the high costs dissuaded a survivor from having an abortion. Deciding whether to have an abortion was part of the survivor’s process to reclaim bodily autonomy. The laws are just making it harder for them to get there.

