As Howard Mielke makes his way down the streets of his tree-lined New Orleans neighborhood toward the Bayou St. John, his walk is careful and deliberate. The canal’s waters are calm and glassy, reflecting the wisps of clouds above, and revealing none of the dangers below where alligators sometimes lurk.
Mielke is a man of habits and, as he does every workday, he makes his way across the canal to the bright red streetcar that awaits the first of the morning’s commuters near the lush gardens of New Orleans’ City Park. At exactly five minutes to 8 a.m. on a steamy September morning, he boards the streetcar and a few minutes later it lurches toward his downtown office at the Tulane University School of Medicine.
It’s the briefest of trips for Mielke on a journey that has stretched decades to try to help save the country’s children from a danger hidden in the soil on which they play.

Mielke has spent four decades investigating the dangers of lead contamination in soil across the country — from Baltimore, Maryland to Minnesota’s Twin Cities to New Orleans, where he has geographically mapped lead soil levels over the course of 20 years. He is an urban geochemistry and health expert who teaches in the department of pharmacology at Tulane University’s School of Medicine.
The result of his life’s work is spread across his office: from awards like the Katrina Heroes commemoration he received from New Orleans in 2015 to the 1984 photograph taped to a file cabinet showing Mielke testifying before the U.S. Senate. The words “Thanks Howard, with your help we’re ‘getting the lead out!’” are scribbled underneath, a note from former Sen. David Durenberger (R-MN).
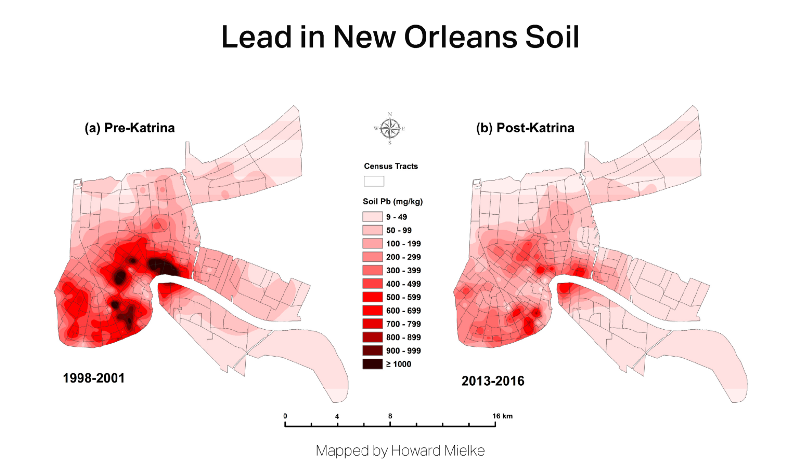
But Mielke has given the most prominent position on his office wall to a large, colorful map of New Orleans he created. It shows the median levels of lead in the city’s soil, illustrated in a range of reds. The highest lead levels, those greater than 1,000 parts per million, are a vibrant crimson—signaling danger.
What’s illustrated so colorfully on the map is not visible to the human eye in the real world.
“You’re always working with invisibles,” he said, pointing to the map, which is peppered with dots and triangles representing childcare play areas and public playgrounds. “The map — nobody sees this on the ground. You wander around, you don’t realize that there’s a mountain of lead downtown.”
The map is the result of countless hours that he and his small team of research associates have poured into collecting dirt samples, testing for the presence of lead, and analyzing the results in order to create a map showing just how pervasively lead has contaminated soil in New Orleans.

Mielke’s work, geographically mapping contaminated soil and documenting the effects on the blood lead levels of children who ingest or inhale these particles, confirms the predictions of a scientist who decades ago broke new ground on lead’s impact: Clair C. Patterson, a California Institute of Technology geochemist.
Patterson pioneered techniques to measure lead levels. By measuring the accumulation of lead within Arctic ice-core samples, he discovered that tetraethyl lead additives in gasoline fuel had contributed significantly to the rise in atmospheric lead levels.
“You wander around, you don’t realize that there’s a mountain of lead downtown.”
In the 1960s and 1970s, Patterson also challenged the notion that existing levels of lead in the environment were normal, and argued that Americans’ blood lead levels were unsafe. His findings subsequently provided key evidence for environmental activists who sought to remove lead from gasoline and reduce emissions.
In a 1980 report to the National Academy of Sciences, Patterson wrote that “Sometime in the near future it probably will be shown that the older urban areas of the United States have been rendered more or less uninhabitable by the millions of tons of poisonous industrial lead residues that have accumulated in cities during the past century.”

Patterson’s research was instrumental in the work that led the government to ban the lead additives, which significantly reduced lead gasoline emissions. But the battle was far from over.
Decades of emissions left a dangerous legacy behind: large deposits of lead particles that remain in the soil today and continue to plague communities with a history of high-density traffic flow.
“It’s a long story and it’s a continuing one, and it would be nice to have an ending to it,” said Mielke.
Cleaning up a crisis
Over the last decade, a growing body of scientific evidence has shown that the harmful effects of childhood lead exposure are far greater than previously thought. Today, the consensus among health experts is that there is no safe level of lead exposure. Studies have also shown that there is no type of intervention that is effective in lowering blood lead levels. In short, prevention is paramount.
Yet the most effective approach to reducing childhood lead exposure — removing the lead from the environment — is a solution that has been largely ignored in favor of simply treating lead-exposed children first, then remediating the problem secondarily, said Mielke.
“We can measure the environment, we can map cities, that’s within our grasp. It’s easy to undertake and do, but we’ve chosen instead to measure blood lead,” said Mielke.
“We can measure the environment, we can map cities, that’s within our grasp…. we’ve chosen instead to measure blood lead.”
Funding, however, is one of the biggest roadblocks to achieving primary prevention, which requires locating sources of exposure in the environment, plus screening communities with high risks of environmental exposure.
“We know where the higher lead levels are going to be. This is not complicated. We know that in the deep interiors of our urban centers that’s where the problem really lies,” said the University of Cincinnati’s Kim Dietrich, director of epidemiology and biostatistics at the university’s College of Medicine.

“Unfortunately, the resources don’t exist or the will probably doesn’t exist to go through these communities and test every home, every flat, every apartment for hazardous levels of lead,” said Dietrich.
The preventative approach also requires pediatricians serving families in these areas to abide by the federal screening laws, said Dietrich. Federal law requires all Medicaid-enrolled children to be tested at 12 and 24 months for lead exposure, but previous research has shown compliance rates are low.
Dietrich recommends targeted screening for children living in high-risk areas at the ages of 6 months, 12 months, 24 months and three years. His research has shown that blood lead levels start to rise when an infant begins to crawl.
Lead screening “should be as done as faithfully as we try to do vaccination immunization. It should be part of the medical regimen for children,” said Dietrich.
The cost of inaction versus the cost of cleanup
The cost of lead remediation on a national scale would be significant. In New Orleans, the soil cleanup projects that Tulane University’s Howard Mielke has overseen target high-risk areas, such as childcare centers, by covering lead-contaminated soil with geotextile fabric and placing a six-inch clean river soil cap atop the fabric.
The geotextile fabric costs about 2 cents per square foot, while the truckload of Mississippi river soil costs about $180 per project, which amounts to $2–4 per square foot. For a 1,000 square foot area the total cost is about $4,000 said Mielke.
There are also soil removal methods known as “dig and haul” that are more expensive at $36 per square foot. The U.S. Environmental Protection Agency has used this technique to remove contaminated soil from urban areas, but at an urban soil workshop last fall, one EPA regional administrator noted the cost savings and effectiveness of Mielke’s approach.
“It costs a ton of money to haul off soil and replace it with clean soil. Howard has done inches instead of feet, and there is no haul away. There is a ripple effect and it is amazing how much change can take place,” said EPA toxicologist Marc Stifelman, according to the meeting summary notes.

When Hurricane Katrina barreled through New Orleans in 2005, it swept away top soils en masse. As a result, the storm left a lower concentration of lead in the city’s soil and has contributed to a “profound” decline in childhood blood lead levels in the city, according to Mielke.
Mielke’s tests show that when the city’s homes were rebuilt, soils with less lead had replaced the contaminated soils. The storm may have also contributed other toxic contaminants such as arsenic, but this is disputed by experts.
“Of course you have to have a hurricane to change the environment,” Mielke said ruefully.
He estimates that a soil cleanup program — that replaces high-lead soil with cleaner low-lead soil — would cost an estimated $12 million for a mid-size city.
On the other hand, the cost of inaction is enormous. In 2002, researchers found that even at low levels of lead exposure, the costs associated with direct medical care and potential productivity losses for lead-burdened U.S. children when they become adults amounts to $43 billion annually. This does not include special education costs or the costs of incarceration.
And economist Elise Gould from the Economic Policy Institute has estimated that the cost for lead paint hazard control just for homes considered to be a significant risk — because the homes had a combination of both lead paint hazards and low income families with children under the age of 6 years — is an estimated $1.2 to $11.0 billion.
Gould also found that the benefits of tackling lead contamination on a widespread scale are substantial given the costs of medical treatment, lost earnings, tax revenue, special education, lead-linked attention deficit hyperactivity disorder cases, and criminal activity.

Every dollar the United States invests in lead paint hazard control results in a return of $17 to $221, or a net benefit of $181 to $269 billion, according to a 2009 study by Gould. The study focused on the 6.9 million young children with elevated blood lead levels in a 2003–2006 national health survey, and excluded other costs such as health care later in life.
“That’s an extraordinarily cost-beneficial intervention, said Bruce Lanphear, a professor of health sciences at Simon Fraser University in Canada. His research has focused on fetal and early childhood exposure to lead and other environmental neurotoxins.
“So the question is, if we know that lead is toxic, that there is no safe level, that it’s associated with the development of ADHD, diminished intellectual ability, diminished academic abilities, hypertension, chronic kidney disease in adults, and it’s cost beneficial, why aren’t we doing more?” said Lanphear.
Failing to map the country’s danger zones
Despite California regulations that clearly state that California’s Childhood Lead Poisoning Prevention Program must identify and target areas where childhood lead exposure is significant, the state has not mapped problem areas.

One state investigation conducted about 25 years ago into both blood lead levels and environmental sources revealed a much deeper problem than is indicated in state or county childhood blood lead data.
The California Department of Public Health, then known as the Department of Health Services, conducted an extensive lead-screening survey of 1,397 children under the age of 6 years and their homes in four California communities: Oakland, Sacramento, Wilmington, and Compton in Los Angeles County.
Of the sampling of children whose blood was tested for lead, Oakland had the highest percentage of children whose levels were 10 micrograms per deciliter (mcg/dL) or higher. The study found that 67 percent of children in Oakland, 32 percent in Wilmington/Compton, and 14 percent in Sacramento had elevated blood lead levels, according to the report issued by the Centers for Disease Control and Prevention (CDC).
Lead paint levels and lead soils were also the highest in Oakland, with 46 percent of soil lead levels exceeding 1,000 ppm. The findings indicated “a high prevalence of elevated [blood lead levels] among children in high-risk communities in California.” The report also noted that because the participating children did not have overt symptoms, without the survey the high prevalence may not have been discovered.
“So the question is, if we know that lead is toxic, that there is no safe level, that it’s associated with the development of ADHD, diminished intellectual ability, diminished academic abilities, hypertension, chronic kidney disease in adults, and it’s cost beneficial, why aren’t we doing more?”
Environmental investigations conducted by the Orange County Health Care Agency in all of Orange County between Jan. 1, 2010 and Jan. 31, 2015 show that 24 percent (17) detected deteriorated lead-based paint as a source. Another 12 percent (two) identified dust, and 18 percent (three) also identified soil as a lead source.
The OCHCA had not analyzed the investigations to search for trends by city or neighborhood, said an agency representative. But the agency says it notifies and raises awareness in at-risk communities via outreach.
“We definitely do make a point of focusing our efforts in those communities where we have higher numbers of positive lead tests,” said David Nuñez, the Orange County Health Care Agency’s family health medical director.
Lead screening “should be as done as faithfully as we try to do vaccination immunization. It should be part of the medical regimen for children.”
Pinpointing lead hot spots is the work Howard Mielke has been doing for decades via his urban soil geochemistry research, which maps lead levels and provides a statistical analysis of the clustering of high lead soil concentrations throughout a neighborhood. It’s a tool that can be used across the country to predict childhood lead exposure, said Mielke.
But Mielke too has encountered funding obstacles to do this geomapping work. He has partnered with the New Orleans public health department to measure childhood blood lead levels, but has struggled to find federal money to measure soil lead levels post-Katrina. To get the work done, he’s tapped his own savings as well as private donations to his nonprofit, Lead Lab.
Mielke believes that the federal agency best equipped to measure soil lead levels is the U.S. Geological Survey, which he said has the mapping and measuring skills to get the job done.
But the Geological Survey’s mission is to survey non-urban areas, which precludes them from measuring in cities, said Mielke. However, the agency’s existing surveys confirm measures of low levels of lead in rural areas, which is useful for urban areas seeking clean soil to replace contaminated soil, said Mielke.

“It provides a really good basis for understanding that every city in the country has available to it soil that can be readily used to change the environment in the city,” said Mielke.
But at a time when the Trump administration is moving to scale back environmental protections, implementing a federal lead contamination survey would likely face roadblocks.
And even if lead hot spots were pinpointed, finding the resources to remediate the soil would also be a challenge.
“Since we don’t have a clean soil act, we don’t have an equivalent to the Superfund sites for residential areas that we do for industrial sites,” said Mielke. “Who would pay for all of the [leaded] gasoline that has been consumed in the U.S.? The real liability is showing up on the children and their future.”

For Columbia University Professor David Rosner, who co-authored the 2013 book Lead Wars: The Politics of Science and the Fate of America’s Children, the issue isn’t whether the United States has the means to address the lead crisis facing communities across the country.
“I always have a problem with the argument that there isn’t enough money,” said Rosner. “That’s a social decision. We make the decision. We have plenty of money when we want to use it for different things.”
He described lead poisoning as the longest running childhood epidemic in American history and an issue that could have been addressed a century ago. But the public ignored the issue, he said.
“The rest of the country basically saw it as an idiosyncratic thing, affecting just a few black kids and Hispanic kids and therefore unimportant,” said Rosner, whose research focuses on public health, social history, and the politics of occupational disease and industrial pollution.
“Lead poisoning is the longest running childhood epidemic in American history.”
“We knew about it, we knew what causes it, we knew where the danger was. There’s nothing about it that’s magic, but we keep studying it,” Rosner said with a wry chuckle. “We just keep studying it and watching it. And it’s terrifying.”
Soil remediation as a national solution
While the United States has failed to meaningfully map its lead epidemic, other countries have succeeded.
A little more than a decade ago, Norway’s environmental protection agency implemented a clean soil program at childcare centers, school yards, and playgrounds across the country, thanks in part to Howard Mielke’s research on New Orleans. The program focused on Norway’s ten largest cities.
Rather than measure blood lead levels to detect lead, Norway tests soils to determine lead contamination and then cleans the soil. Norway also doesn’t require proof that a child has been lead-poisoned in order for the government to offer assistance, said Mielke. Having a lead-contaminated environment is enough to trigger action.
Norway’s soil guideline for children’s play areas was 100 parts per million in 2011, then was lowered to 60 ppm, according to Mielke. He recommends a soil standard of 40 ppm. The federal standard set by the EPA for children’s play areas is 400 ppm.

Many U.S. urban centers have median lead soil levels above 100 ppm, Mielke noted in a 2011 paper, and his New Orleans research has shown that communities with a median soil lead level less than 80 ppm would generally prevent children from having blood lead levels higher than 10 micrograms per deciliter.
But the CDC recommends public health intervention for young children with blood lead levels above 5 mcg/dL. This means that soil lead guidelines must be significantly lower than the current federal standard and even lower than 80 ppm, according to Mielke.
One of Mielke’s solutions to clean urban soils is to cover contaminated dirt with soil that’s removed from new suburban developments, which tend to have lower lead levels.
In New Orleans, Mielke has used his geomapping research to pinpoint childcare centers in neighborhoods with high levels of lead. He and his research team then collect soil samples from the center’s play areas to measure the lead levels later in his laboratory, but he arranges to have a contractor on site to immediately add a clean layer of soil so that the childcare center doesn’t have to await the lead test results.
Mielke sources soil from the Mississippi River, which he says carries “the best farmland in the world past our door step at a rate of 300 tons per minute.” The soil contains lead at 5 parts per million, far lower than the 500 to 1,000 ppm soil Mielke finds throughout New Orleans.

“I’m concerned about that very top layer of soil because the children are playing in the top layer,” said Mielke. “You don’t have to dig out two feet of soil to have a clean play area.”
Under Trump’s ‘deregulation’ push, lead protections could be rolled back
Researchers such as Mielke have focused on transforming children’s outdoor environment, but more work is needed to address the indoor areas where children live as well.
Legal experts told ThinkProgress that federal, state, and local governments have failed to create housing regulations and policies that are stringent enough to prevent childhood lead exposure from occurring both in public and private housing.
But the Trump administration has directed the Environmental Protection Agency to significantly slash its budget and issued a presidential order that federal agencies lower regulatory burdens. Environmental, health, and legal advocates fear that the EPA will relax standards and repeal programs, rather than strengthen lead protections for children.

Emily Benfer, a faculty member at the Loyola University Chicago School of Law described the potential repeals and changes that the EPA is considering to lead programs and regulations in the Toxic Substances Control Act as “catastrophic.”
Benfer has spent half a dozen years working in collaboration with health providers, legal aid workers, and law students to help low-income families battle toxic living conditions in lead-contaminated Illinois neighborhoods.
“If you relax the lead hazard standards in paint, dust, and soil — major lead hazards will go undetected and that will result in permanent brain damage for millions of children in the future,” said Benfer. “This is not the time to dismantle them.”
Loyola’s Health Justice Project, which Benfer founded and until recently directed, was part of a coalition of organizations that petitioned the U.S. Department of Housing and Urban Development in early 2016 to update public housing lead regulations.
One outdated regulation, for example, allowed public housing authorities to compel landlords to make lead repairs only after a child’s blood lead level reached 20 micrograms per deciliter—four times higher than the CDC’s current actionable level of 5 mcg/dL.
“If you relax the lead hazard standards in paint, dust, and soil — major lead hazards will go undetected and that will result in permanent brain damage for millions of children in the future.”
Last year in its written response to the coalition, HUD outlined the agency’s plans to update its definition for elevated blood lead levels to align with the CDC’s level. Earlier this year, HUD followed through when it published an amendment to the Lead Safe Housing Rule, which applies to federally-owned housing or those who receive federal housing assistance.
On April 1, HUD also began enforcing more stringent requirements for government agencies who receive federal grants that pay for lead-based paint hazard testing and abatement in homes. The agency lowered some dust hazard action levels and tightened standards for abatement.
“This is not the time to dismantle” regulations.
But even as HUD has made advances, the Environmental Protection Agency has lagged behind in updating its own regulations. Advocates say the EPA’s shortcomings have far wider implications: Federal agencies such as HUD as well as states and cities across the country defer to the EPA standards when setting their own lead regulations and policies.
The American Academy of Pediatrics described the regulations as “obsolete” last year in a report on preventing childhood lead toxicity. The academy also noted one study that found that under the EPA’s current floor hazard standards for lead dust measured after abatement work is completed, 50 percent of children were estimated to have a blood lead level of 5 micrograms per deciliter or higher.

“In other words, at the current dust-lead hazard standards, half of children in families informed that their home does not contain a dust-lead hazard would nevertheless develop elevated blood lead levels,” attorneys for the environmental law organization, Earthjustice, stated in a lawsuit filed against the EPA on behalf of eight organizations across the country.
“I think there’s clearly enough evidence right now for them to move forward to strengthen the standards, because we know now what we didn’t know as clearly in 2001 when the standard was adopted, that there is no safe level of lead,” said Eve Gartner, a litigator at Earthjustice where she oversees efforts to protect people from toxic chemicals in the organization’s Healthy Communities Program.
“At the current dust-lead hazard standards, half of children in families informed that their home does not contain a dust-lead hazard would nevertheless develop elevated blood lead levels.”
If the EPA decides to revise the standards, the agency indicated in its response to the Earthjustice lawsuit that it could take as many as six more years for the new standards to take effect.
“We just think this is egregious, that something as basic as updating the standard so that it’s health protective would take them from 2009 to 2023,” said Gartner, referring to a citizen petition sent to the EPA administrator in 2009 asking the agency to make the standards more stringent.
But there’s a possibility that strengthened standards may never take effect at all: Trump has repeatedly promised the federal agencies will face extreme “deregulation.” The EPA—and its lead guidelines—are likely targets.
Benfer is particularly concerned with the possibility that the EPA might relax lead dust standards, given that research has shown that the current standards are not effective at protecting children from lead exposure.

When the government fails to properly identify lead hazards in housing, and standards are not consistent across agencies this allows children to continue to be the “canary in the coal mine,” said Benfer.
Currently, the federal Residential Lead-Based Paint Hazard Reduction Act doesn’t require homeowners to remediate a lead source. Legal experts also say the law may incentivize property owners to remain in the dark about potential lead contamination to avoid having to disclose the issue.
One option would be to require all homeowners to screen their property for lead hazards and address the problem before a new occupancy, said Simon Fraser University’s Bruce Lanphear in an interview.
“The emphasis should be on screening the homes before the child is poisoned, but we haven’t been willing to do that,” said Lanphear, an epidemiologist and professor of health sciences.
“The emphasis should be on screening the homes before the child is poisoned, but we haven’t been willing to do that.”
Few states require pre-rental lead-free certification, as Maryland and Maine do, said Benfer, noting that these states have had success with these programs. In 2015, a Maryland law went into effect requiring all rental properties built before 1978 — when the federal government banned lead paint for residential use — to have lead paint inspections prior to tenancy changes.
“They did not lose affordable housing, they did not have a loss in rental units, and they were able to actually clean up a lot of the lead hazards,” said Benfer.

Last year, Maryland launched a new campaign to combat childhood lead poisoning and declared the entire state at risk for lead exposure for children born on or after Jan. 1, 2015. Now, under the state’s universal testing plan all 1 and 2-year-olds born after that date must be tested for lead.
“This is definitely going to require a commitment on the part of our federal and local governments to address the issue and commit funding to it,” said Benfer. “If we spend our effort…on the systemic elimination of environmental lead exposure connected to housing and the gas emissions… we could actually eradicate lead poisoning in the United States.”
Schools have a role to play in helping lead-burdened children early on
The University of Cincinnati’s Kim Dietrich believes that school systems can also play a role in identifying children who have been exposed to lead contamination. He co-authored a report published by the CDC in 2015 that outlines the signs that indicate lead exposure could be one of the factors affecting a student’s academic performance.
“Lead doesn’t have a highly specific behavioral signature so just because you have a child acting out in your class, having difficulty learning to read or doing calculations… you can’t be certain that that’s due to lead,” said Dietrich. “But the fact is that many lead-exposed children do tend to show these particular types of behavioral problems.”
“We could actually eradicate lead poisoning in the United States.”
A proper diagnosis could also reduce the risk that families face that their child will be labeled a troublemaker. Dietrich discovered in Flint, Michigan that children exposed to lead were being described as “lost” or “unredeemable.” That’s nonsense, he said.
Recent findings from a study of lead-burdened Rhode Island children could be a powerful tool for educational leaders who not only want to address school disciplinary issues, but hope to improve educational outcomes such as test scores, says another expert.
“If you care about educational outcomes you might actually start thinking about things like housing and air pollution,” said study co-author Anna Aizer, a Brown University economics professor.
“If you care about educational outcomes you might actually start thinking about things like housing and air pollution.”
Rather than rely solely on blood lead tests, Aizer said that measuring lead in the environment could provide more accurate assessments of the presence of lead in a child’s surroundings.
“An obvious thing is to look at soil in and around schools and playgrounds, places where kids are. It seems like the obvious starting point,” said Aizer.
One lead soil study in New Orleans found although the amount of soil lead on elementary schools followed the same general pattern as soil lead on residential properties, the schools only had a fraction of the lead compared to the homes, where preschool children — the most vulnerable to the neurotoxin’s effects — are most likely to play.

Although the costs of environmental lead remediation are high, they pale in comparison with the costs associated with student behavioral and disciplinary issues, as well as juvenile delinquency, said Aizer. Nationally, the estimated cost to detain a juvenile in detention for one year is $100,000.
“So to not consider the cost savings associated with these remediations, which can be extremely high, is really foolish,” said Aizer.
Community action and the role of the courts
Columbia University’s David Rosner said he’s fielded many more calls from communities across the country wanting to take action since the Flint, Michigan lead water crisis became public. Some communities are filing lawsuits in an attempt to hold the petroleum and paint industries responsible for paying for environmental cleanup as well, he said.
“Communities that are politically organizing around [lead accountability] are going to be the ones who really make change,” said Rosner.
Rosner testified in one such public nuisance lawsuit filed in California by ten counties and cities against three paint manufacturers. The judge ordered the companies to pay $1.15 billion into a fund to conduct lead inspections and remediation inside homes. That decision is on appeal.
“Communities that are politically organizing around [lead accountability] are going to be the ones who really make change.”
Even when a lawsuit fails, Rosner said, community awareness about the dangers of lead increases and results in action.
“…People become more aware of lead in the community and begin to understand it’s not just the industries’ responsibility, but society’s responsibility,” said Rosner.
Proactive communities can also push legislators to address the lack of health care data on children with the lowest levels of lead exposure, under 5 mcg/dL. Low blood lead levels are associated with a host of issues such as lowered IQ levels, attention-related behaviors, and poor academic achievement, according to the accumulated body of scientific evidence.
“It’s not just the industries’ responsibility, but society’s responsibility.”
Lead paint exposure tends to get the most attention. That’s because when children ingest lead via paint chips or dust this can lead to very high blood lead levels, which also result in overt symptoms such as vomiting, said Howard Mielke. So children with the highest lead exposures land in the hospital, but the majority of children being exposed to lower levels of lead will never show up in the emergency room, he said.
“They’re not in the hospital, but they’re still getting exposed,” said Mielke. “It’s a very subtle kind of disease.”

This is something that Mielke learned first-hand in the early 1980s when his own daughter was exposed to contaminated soil lead in her childcare center, which was near a major freeway. During a routine check up, Mielke discovered that his daughter, then a toddler, had a blood lead level between 10–15 mcg/dL.
“I tried to prevent her from putting her hands in her mouth, and it was a total losing battle,” said Mielke. “It became very clear to me that I had to change her environment.”
Mielke discovered that the state’s licensing inspection focused on the conditions inside the childcare center. But it was outside that the children faced an invisible danger as they played in a sandbox and in the yard, where Mielke tested samples and found hazardous levels of lead in the soil.
“They’re not in the hospital, but they’re still getting exposed… It’s a very subtle kind of disease.”
Mielke replaced the sand, and placed outdoor carpet on the soil around the sandbox. Shortly after he did this, his daughter’s blood lead levels dropped by half. The experience spurred him to action.
“If this is happening to my child, it must be happening to other children. So the question is how many children in the Twin Cities are getting lead poisoned,” said Mielke, who lived in Minnesota at the time of his daughter’s lead exposure. His research in Minnesota showed that inner city children were being excessively exposed to high levels of contaminated soil.
“If this is happening to my child, it must be happening to other children.”
His testimony was pivotal during a U.S. Senate committee hearing on reducing lead in gasoline. Thanks in part to Mielke’s work and willingness to speak out, Congress moved to implement the leaded gasoline phase-down more quickly, on Jan. 1, 1986.
More than anyone, Mielke would have liked the story of lead contamination to have ended there. But the deeper scientists dig the more they discover that the effects of lead are far worse than what was originally believed. If other U.S. cities were geographically tested and mapped the way Mielke has done in New Orleans, the extent of the contamination from gasoline emissions, paint, and other sources would be clearer, said Mielke.

For now, Mielke and his research associates are working methodically to clean the yards of childcare centers and parks in New Orleans. Mielke visited one of those centers on a September morning as the children played in the backyard.
Preschoolers crowded around a miniature kitchen and went about scooping fistfuls of dirt, leaves and grass on to tiny plastic plates. Taking turns, they slid their plates full of dirt into the play oven to “bake” their pies.
Dirt was everywhere: smudged on their pants and shirts, on their faces and hands. But the children’s caretakers weren’t alarmed. Nobody warned the children to keep away from the soil. Standing nearby, Mielke just observed and smiled knowing that the children weren’t in danger.
Back at his office, he keeps a file of photographs of these childcare centers as examples of what can be done.
“It’s changing the world one yard at a time,” said Mielke. “You’ve got to start someplace.”

This project was made possible through the generous support of a community health reporting fellowship from the International Center for Journalists.
